Behavioral Health
Living well means taking care of your physical health and your mental health
Your behavioral health benefits provide treatment for mental health and substance use disorders. Behavioral health providers include therapists, psychologists, and psychiatrists.
What services are covered?
Your mental health and substance use disorder benefits may include:
- Sessions with a therapist, psychologist, or psychiatrist.
- Treatment follow-up and aftercare.
- Other inpatient and outpatient services that are medically necessary.
How do I get help?
Simply call the Behavioral Health benefits number on the back of your Health Net ID card. Our staff, including customer service reps and licensed clinical Care Managers, are available to take your call. They can help you:
- Answer questions you have about your benefits.
- Find a behavioral health provider for you based on your needs.
- Get help right away if you are experiencing a crisis or emergency.
- Schedule an appointment if you are having difficulty.
Find a therapist or psychiatrist or call the Behavioral Health Benefits number listed on your Health Net ID card. You won't need approval for outpatient appointments.
This is only a summary of benefits. For details about copayments, deductibles, exclusions and member/dependent eligibility, please refer to your plan documents.
Need help finding a behavioral health provider?
- For outpatient office visits for therapy and/or medication management with an in-network provider, no prior authorization is needed.
- For help, contact Customer Service – 800-663-9355 – Monday-Friday, 8:00 a.m. to 8:00 p.m. Pacific time. A Customer Service Representative will assist if you'd like help finding a provider with availability. Health Net will outreach to providers on your behalf and will contact you with the soonest appointment available.
Please note: routine appointments with an MD/psychiatrist may take up to 15 business days, and an appointment with a therapist may take up to 10 business days.
If you or a family member is feeling suicidal or experiencing another type of mental health emergency, go to the nearest ER or call 988.
You and your covered family members can use behavioral health benefits for medically necessary behavioral health services, as well as treatment for substance abuse.
- No prior authorization required for:
- Outpatient therapy or psychiatric care, whether delivered in person or via telehealth
- Prior authorization is required for:
- Intensive treatment programs delivered on an outpatient basis
- 24 hour in-patient treatment or residential care
- Applied Behavior Analysis for children with Autism Spectrum Disorder
Download Behavioral Health Benefits Brochure – English (PDF)
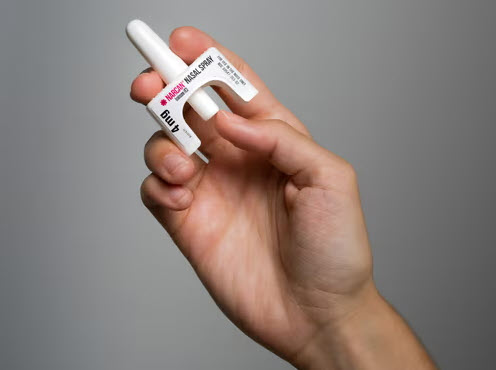
Stop Opioid Overdoses and Help Save Lives with Naloxone
Opioid overdose is an increasing problem in California. Opioid drugs are used to control pain. Taking too much of a prescription painkiller such as Norco, Vicodin, morphine, fentanyl, or street drugs laced with fentanyl or heroin can lead to drug overdose, and death.
Naloxone is a life-saving medication used to reverse a drug overdose from opioids. It can be given via a nasal spray or injection or auto-injector into a major muscle. You can purchase Naloxone in nasal spray form at local pharmacies. To learn more about your risk for overdose, talk to your doctor or pharmacist. Learn more about Nalaxone.
- Teladoc Mental Health (Digital Program). This program is a confidential online resource, personalized to help improve your mood. The program's self-help tools are designed to help empower you to become — and stay — mentally and physically healthy. Sign up for this program at Teladoc Health. Learn more about the Teladoc Mental Health Digital Program:
- UCLA Mindful Awareness Research Center (MARC) and Guided Meditation Podcasts. Each weekly podcast has a different theme and offers a new daily life practice, guided meditation, silent practice time, and closing comments.
- Krames Online Health Library – Not sure what do when you have a cold or the flu? Or how much sunscreen to apply? Or what to do if you're expecting a child? Search for these topics and more on this health library.
- Child Anxiety – You and your child can learn to manage anxiety. Even in tough times you can bring on the calm.
Resources and Hotlines
- 988 Suicide & Crisis Lifeline – provides a direct connection to the National Suicide Prevention Lifeline's network of over 200 local crisis centers which provide 24/7 support to people in suicidal crisis, emotional distress, or substance abuse crisis.
- 211 – available 24/7 for assistance finding food or basic needs
- 24-hour Domestic Violence Hotline: 800-799-7233 or thehotline.org (click Chat Now)
- Disaster Distress Helpline: 800-985-5990 (TTY 800-846-8517) or text TalkWithUs to 66746
- National Parent Helpline 855-427-2736 – Monday-Friday 10:00 a.m. to 7:00 p.m. Pacific time
- Substance Use
- SAMHSA National Helpline: 800-662-HELP
- Mental Health
- NAMI California: 800-950-NAMI from 7:00 a.m. to 3:00 p.m. or email info@namica.org
- California Peer-Run Warm Line: 855-845-7415
- LGBTQA+
- Trevor Project: 866-488-7386 or text START to 678678 for 24/7 information and suicide prevention resources for LGBTQ youth
- Lesbian, Gay, Bisexual and Transgender National Hotline: 800-273-8255 from 1:00 p.m. to 9:00 p.m. for support, information or help finding resources
- CalHOPE: 833-317-HOPE (4673) – CalHOPE builds community resiliency and helps people recover from disasters through free outreach, crisis counseling, and support services. Services include: Individual and Group Crisis Counseling and Support, Individual and Public Education, Community Networking and Support, Connection to Resources
